+1(209) 348-9544
order@myessayservices.com
+1(209) 348-9544
order@myessayservices.com
![]() Are you in High School, College, Masters, Bachelors or Ph.D and need someone to help write your paper? All you need is to ask for research paper help written by a specialist in your academic field. When you buy an essay online from us, we offer you an original, nil plagiarized and unique paper written by a dedicated writer who is PhD or Masters qualified. MyEssayServices.com is an experienced service with over 9 years experience having delivered over 83,000 essays over the years.
Are you in High School, College, Masters, Bachelors or Ph.D and need someone to help write your paper? All you need is to ask for research paper help written by a specialist in your academic field. When you buy an essay online from us, we offer you an original, nil plagiarized and unique paper written by a dedicated writer who is PhD or Masters qualified. MyEssayServices.com is an experienced service with over 9 years experience having delivered over 83,000 essays over the years.

Advanced practice nursing has evolved over the past years. With many areas of specialty in nursing, there is bound to be intra profession conflicts. However, many nurses are well educated on ethical behaviors such as positive job relationships. In nursing practices, there are high levels of interproffessional relationships aimed at enhancing quality patient care.
I chose family nurse practitioner profession because it entails a wide working environment. For instance, one can work at schools, homes, hospitals, and community health centers among other working environments. In addition, after a productive term of job experience, one can open his or her own offices where state laws are favorable. Further, working with families creates an understanding and a professional relationship, which enhances better understanding (Hamric, Spross & Hanson, 2009).
Potential Inter-professional Conflict Issues
There are various types of APNs; acute care nurses, primary healthcare nurses and clinical nurse specialists. In the working environment, decision making roles may conflict among these nurse practitioners. Consequently, nursing role limitations may also create an inter profession conflict. Most colleges only restrict certificate nurses practice, but they do not offer limitations for advanced nurse practitioners (DeNisco & Barker, 2013). This may lead to a conflicting environment among various nurse practitioners.
How to avoid conflicts
In order to avoid conflicts, I would create a participative leadership style. This will bring colleagues together as a team. Furthermore, I would create a leadership strategy where all conflicts will be reported and solved through a particular procedure. Consequently, state laws regulate the areas of practice for nurses. Therefore, these state laws would help reduce conflict levels among nurses.
In most healthcare institutions, there are boundaries on various nursing roles. These boundaries create an efficient working environment with low chances of interprofession conflicts. Similarly, in some states nurses are prohibited from administering drugs unless authorized by a doctor. Certain laws limit interproffession conflicts. It is also important to respect other professions in your working environment and enhancing teamwork in order to achieve quality patient care (Trodd & Chivers, 2011).
References
Hamric, A. B., Spross, J. A., & Hanson, C. M. (2009). Advance practice nursing: An integrative approach. St.Louis, MO: Saunders Elsevier.
DeNisco, S., & Barker, A. M. (2013). Advanced practice nursing: Evolving roles for the transformation of the profession. Burlington, Mass: Jones & Bartlett Learning.
Trodd, L.,& Chivers, L. (2011). Interprofessional working in practice: Learning and working together for children and families. Berkshire, England: Open University Press.
 Advanced nursing practice is one of the most demanding professions. In my weekly, orientations, researches and presentations, I was able to employ my theoretical knowledge into practice. The assessment of the final paper enabled me to fully diagnose patients and understand the medical environment that nurses work.
Advanced nursing practice is one of the most demanding professions. In my weekly, orientations, researches and presentations, I was able to employ my theoretical knowledge into practice. The assessment of the final paper enabled me to fully diagnose patients and understand the medical environment that nurses work.
First, the process enabled me achieve full diagnostic knowledge of patients in a clinical situation. The weekly case studies involved deep researches and physical assessments of various patients. This expounded my nursing knowledge and experience. I was able to deal with patients who presented with emergencies. My encounter with these patients shaped my nursing experience. Further, I was able to learn the value of evidence-based practice to fully diagnose patients. In most patient situations, I was required to work collaboratively with other medical practitioner. For instance, I ordered for various tests in the laboratory, sometimes I asked for help from the nurse educator and I other specialists such as therapists.
I learned the basic critical thinking skills required to evaluate the level of patient preference towards various diagnoses. For instance, most patients have a phobia for undergoing a surgery. Thus, in order to counter this phobia, it was necessary to educate these patients or to refer them to a counselor in order for them to accept the treatment.
Moreover, I learned that one of the most important aspects of treatment is patient education. Patient education should also include the patient’s family and support system. For patients with low or no support system, more support came from me during the recovery process. This was in order to evaluate the success of diagnosis first hand. In addition, weekly calls and regular visits were necessary after admission of the patient (Terry, 2012).
While diagnosing chronic illnesses, one should first begin with primary acute care (Buttaro, Trybulski, Bailey & Sandberg-Cook, 2013). After primary care, the results found, from both the patient and the nurse interpretations, should be diagnosed differently in order to assess the level of infection. However, while diagnosing chronic illnesses I learned that it was vital monitoring and managing the disease condition.
The first major experience during the weekly rounds was the formation of a patient care plan. The patient care plan presents the necessary information pertaining to the patient in question. Further, it presents the current diagnosis of the patient, which needs to be monitored as well. In addition, the care plan enables one to educate the patient using accurate information.
Depression
Apart from disease diagnosing, I learned that it was necessary to evaluate the emotional condition of the patient. Emotions such as stress and depression may lead to slow progress of the patient. Thus, in my medical experiences I learned that it was necessary to evaluate the level of depression or other distractions that may hinder the patient’s progress. The collaborative help of a stress therapist would enable the patient acquire more confidence and become positive with their healing process (Buttaro, Trybulski, Bailey & Sandberg-Cook, 2013).
Hypertension
Hypertension is one of the most common diseases presented during emergency situations. However, I learned that not every crushing chest pain is caused by hypertension. Thus, patients who present themselves with chest pains and they have been previously diagnoses with hypertension required more lab tests and imaging tests to establish the real cause of the condition. However, if hypertension was detected, it is important for the medical practitioner to engage the patient in healthy practices and options other than mere drug prescription. This would solve the condition in the long run. For instance, in order to improve the eating habits of a hypertension patient, the help of a dietitian would provide beneficial help (Buttaro, Trybulski, Bailey & Sandberg-Cook, 2013).
Hypercholesterolemia
Hypercholesterolemia presents itself during increased activity rate. However, while diagnosing the condition various cardiac tests should be conducted. Further, the diagnosis should begin with primary acute care, which should involve a blood test. In order to fully treat the disease, the medical practitioner should provide the necessary patient education regarding the right feeding habits and the ideal physical activities that the patient should engage in.
Urinary tract infections or malfunctions
Urinary tract infections are also common and they require keen observation in order to conclude the cause of the condition. For instance, imaging tests and organ testing would be necessary to establish the cause of the condition. Further, the medical practitioner should assess the patient on the pain patterns (Terry, 2012). This would help the medical practitioner during the diagnosis.
Weekly rounds and my final project improved my nursing practice. This is through the challenges posed by the tests. Weekly rounds provided for random patient test that were quite tactful. For instance, the gout and angina tests shaped my nursing knowledge regarding the conditions. Further, the difference in patient situations presented a nursing challenge that added on to my nursing knowledge. For instance, there were instances where the level of diagnosis did not fully treat the condition. For instance, in cardio-vascular diseases, the patients mostly complained high level of pains. This required the collaborative help of pharmacologists to stabilize and manage the pain levels without paving way for drug dependency.
References
Buttaro, T., Trybulski, J., Bailey, P. P., & Sandberg-Cook, J. (2013). Primary care: A collaborative practice (4th ed.). St. Louis, MO: Elsevier Mosby.
Hamric, A. B., In Hanson, C. M., In Tracy, M. F., & In O'Grady, E. T. (2014). Advanced practice nursing: An integrative approach.
Terry, A. J. (2012). Clinical research for the doctor of nursing practice. Sudbury, MA: Jones & Bartlett Learning.
Nursing entails a wide range or practices including primary care, education, administration and research. All of these specialties create a complete and effective working environment. For instance, some specialties such as family nurse practice engage in full primary care. Their roles involve providing the necessary patient care in almost all environments. Further, they can deal with patients of all ages. On the other hand, nurse administrators are responsible for ensuring full efficiency of their healthcare centers. Their roles include supervising, managing and implementing policies among other leadership roles.
Advanced nursing practitioners can also specialize in education. They are referred to as nurse educators. Their scope of practice widely entails research and high levels of learning. This is to ensure they are capable of educating other nurses with proper nursing knowledge and practices. Advance nurse practitioners who specialize in research (nurse informaticists), participate in processing information within a clinical environment. Their roles include processing information, which relates to patient care. This includes data on patients, information of new healthcare practices and ensuring they provide other nurses with the right information pertaining healthcare practices.
The differences in the corecompetencies of the various advanced nursing specialties involve collaboration, coaching, clinical judgment, caring practices and clinical inquiry. For instance, mainly clinical practitioners such as family nurse practitioners possess caring practices competencies. On the other hand, nurse educators participate in coaching other nurses. Consequently, nurse administrators offer clinical judgment while nurse informaticists offer clinical inquiry. These competencies are used collaboratively to create an efficient working environment (Hardin & Kaplow, 2004).
The Canadian healthcare system is different from the U.S healthcare system in many ways. For instance, the Canadian system is a public system whereas the U.S healthcare system more of a private system. The access and availability of healthcare services is more available to Canadian citizens that it is in U.S. This is because of the healthcare insurance systems in U.S where 1 out of 5 citizens are insured. This leaves out citizens who cannot afford insurance.
Further, in Canada the degree of consumer choice is low because of the government’s investments in the public healthcare systems. Thus, consumers enjoy easy access to public healthcare services. Consequently, in U.S healthcare there is a high degree of consumer choice due to the high numbers of available private healthcare institutions. This creates high levels of competition in the U.S than in Canada. Further, in U.S there are high levels of Advanced Nurse Practice due to the wide specialization of many private healthcare centers (Baker, 2008).
I engaged my colleagues in a discussion on what thought were the main challenges in the U.S healthcare system. Adding up their responses into one, they admitted that U.S had one of the best healthcare infrastructures in the world; the problem is that healthcare services are quite expensive for average citizens. Thus, this limits the equality of healthcare access among all citizens.
Although the U.S enjoys quality levels of healthcare infrastructures, the government should ensure the access and availability of medical services to the poor citizens. Further, there is a high degree of consumer choice but this is only available for the financially capable, mostly those insured. Therefore, the government should consider improving its public healthcare systems in order to reach the poor systems who are not insured (Longman, 2012).
The changes in healthcare aimed at improving the quality of healthcare systems must aim; the effect of the condition of individual’s and population’s health, strong academic research to improve the outcomes of healthcare, patient centered healthcare, technical merit and stakeholders and patients’ engagement (Hardin & Kaplow, 2004).
An example of a successful change in healthcare systems is the Canadian healthcare systems. Researchers conducted by the Toronto University Health Network paved way for positive changes. The university and other bodies involved in change research and implementation, set goals and determined the efficiency of the changes. Thus, the Canadian healthcare system is now more efficient and better suited to patient care than before (Baker, 2008).
According to many state laws, nurse practitioners are responsible for their practices. Therefore, their specialty of nursing practice should be done with care and good professional knowledge. For instance, I asked my fellow nurses what were their main challenges in Advanced Nurse Practice. Most of them acknowledged that their advanced nursing education in different colleges differs in some perspectives. Thus, this may create differences in how nurses practice. Therefore, it is vital for nurse educators to establish a common way of educating nurses. This will improve their working efficiency. Further, nurse administrators should ensure nurses work efficiently, through proper leadership skills.
Further, many clinical institutions have their cultural practices. Thus, the cultural practices alter the competency levels of some nurse practitioners who adjust their skills towards the cultural practices. Similarly, ethical standards limit the scope of practice for nurses. The current patient care focuses on providing patient care services that satisfy patients. Thus, healthcare is nowadays centered on patient satisfaction, which limits the scope of practice for nurses as patients’ are legally allowed take or refuse medication (Tracy, 2008).
Participative leadership is essential in advanced nursing practice. This is because it promotes teamwork, and it engages everyone in the clinical environment. Further, it allows effective communication among nurses because they are able to consult each other in different situations. In addition, participate leadership encourages a collaborative working environment, which improves the quality of patient care (Hamrick, Hanson & Spross, 2009).
There are various models, which have been initiated to improve the quality of patients care. One of the most effective models is the evidence-based practice model. It enables nurses avoid ethical malpractices and it enhances patient care. It also paves way for change in nursing practices in order to satisfy patients’ needs (Hamrick, Hanson, Tracy & O’Grady, 2013). In addition, health committee boards are essential in improving leadership in clinical institutions. Further health committee boards, discuss arising issues, which are hard to solve. This engages the public and nurses in problem solving. Apparently, most of the scholarships available in the U.S are merit based. Thus, one has to achieve the standards required by the giver of the scholarship.
Advanced practice nursing makes the patient’s problems the nurse’s problems as well. Thus, nurses should engage in the best nursing practice with an interest of achieving the best quality of patient care. Evidence-based practices have enhanced nursing practices up to the ethical standards required. Advanced nursing practice specialties pave way for implementation of healthcare policies effectively.
Collaboratively working with the Technology Research Centre (HITRC), technological changes are easily adjusted to suit various health systems. The Institute for Health Improvement (IHI) enables health systems initiate new and more advanced technology by initiating healthcare models.
References
Longman, P. (2012). Best care anywhere: Why VA health care would work better for everyone. San Francisco: Berrett-Koehler Publishers.
Baker, G. R. (2008). High performing healthcare systems: Delivering quality by design. Toronto: Longwoods Pub. Corp.
Hamric, A. B., Spross, J. A., & Hanson, C. M. (2009). Advance practice nursing: An integrative approach. St. Louis, MO: Saunders Elsevier.
Hamric, A. B., Hanson, C. M., Tracy, M. F., & O'Grady, E. T. (2014). Advanced practice nursing: An integrative approach. St. Louis, MO: Saunders Elsevier.
S. Hardin, R. Kaplow. (2004). Synergy for Clinical Execellence: The AACN Synergy Model for Patient Care. Aliso Viejo, CA: American Association of Critical Care Nurses.
Tracy, M.F. (2008). Direct clinical practice. In Hamric, AB, Spross, JA, & Hanson, CM. Advanced practice nursing: An integrative approach. 4th ed. St. Louis: Elsevier.
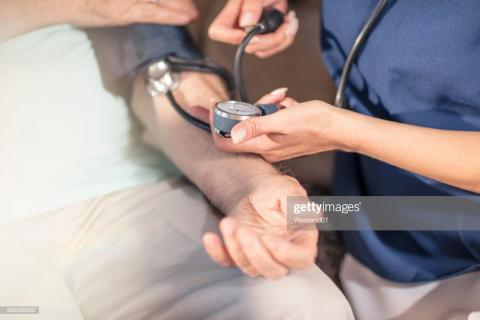 The advanced nursing practice involves high competency levels. Work experience and good job character are essential apart from the basic entry-level education. Work discipline is vital in order for nurses to accomplish the best patient care practices.
The advanced nursing practice involves high competency levels. Work experience and good job character are essential apart from the basic entry-level education. Work discipline is vital in order for nurses to accomplish the best patient care practices.
Family nurse practitioners have a huge role to play in implementing proper patient care. The advanced nursing education may not cover all the aspects required in a clinical setting, work experience is very important. For instance, in the clinical environment, nurses can establish other areas of interest different from their specialty, through experience. Some undergraduate nurse practitioners have developed better working skills and roles through practice. Although this may create intra profession conflicts, it is important to respect their decisions due to the experience they have (Hamric, Spross & Hnason, 2009).
However, there can emerge limitations to the changing of roles. While other nurses increase their working skills potential through experience, this may create intra professional conflicts. According to research, intra professional conflicts can be avoided by proper consultancy and teamwork (Robert, Lindsay & Bobbie, 2012).
What is important for nurses in a clinical setting is work efficiency. Good ties with other professions, such as the doctor, create the best working environment where the patient care needs. However, nurse practitioners can also engage in further certificate studies, which will improve their working skills (Kelly& Matthews, 2001). For instance, in my junior level, I worked as a technical assistant in the emergency unit. As a family nurse practitioner, I can perform wide range of medical services such as delivering acute patient care besides mere technical practices. This way, I can work in multiple environments.
Work experience is important in determining what nursing specialty to pursue. Prior experience in the nursing practice gives one a better decision-making basis on what to specialize. For instance, I chose family nurse practice because it entails wide level of practice.
References
Hamric, A., Spross, J., & Hanson, C. (2009). Advance practice nursing: An integrative approach. (4th ed., p. 96). St. Louis : Saunders elsevier.
Robert Lucero, Lindsay Rauch, Bobbie Berkowitz. (2012). Nurse Practitioner Workforce. Nurse Econ. 2012;30(5):268-274
Kelly, N., & Mathews, M. (2001). The transition to first position as nurse practitioner. Journal of Nursing Education, 40(4), 156-62
Browse More Essay Topics 24/7/365 Support 11+ Yrs in Essay Writing Pay for Quality not Quantity Score that A+ Grade
Affordable Papers
Research Paper for Sale
Cheap Research Papers
Buy Term Papers
Buy Research Paper
Write My Paper
Buy an Essay
Cheap Essay Writer
Write my Essay
Thesis Help
Dissertation Help
Paper Writing Service
Pay for Homework
Pay for Research Paper
Do My Essay for Me
Pay for Essay
College Papers for Sale
Do My Homework for Me
College Essays for Sale
Buy Research Papers Online
Buy College paper
Client: "(Berlin, G.K., CA)"
Topic title:"Leadership shortfalls in Blue Chips"
Discipline: "Economics"
Pages: 5, (APA)
" Awesome, the writer delivered it as required by the professor. They also sent me a plagiarism & grammar report Wow!. I was worried about how the essay would turn up but this is exactly what wanted. Thank you and will be back with a longer essay"
Accounting Research Papers
Business Research Papers
Communication Research Papers
Computer Science Research Papers
Economic Research Papers
Film Studies Research Papers
Finance Research Papers
Geography Research Papers
History Essays
Psychology Research Papers
Political Science Research Papers
Nursing Research Papers
Mathematics Essays
Management Essays
Literature Essays
Law Essays
World Affairs Essays
Technology Essays
Sociology Essays
Science Essays
Religion Essays
+1(209) 348-9544
Terms
Privacy
Sitemap
Frequently Asked Questions
0% Plagiarism Guarantee
Money Back Guarantee
Revision Policy
